This year marks the tenth anniversary of Direct Access, a significant milestone within dentistry that enhanced the scope of clinical activities across Dental Care Professionals (DCPs). In the preceding years, before Direct Access was introduced, the General Dental Council (GDC) commissioned a research project and literature review.
An overwhelming amount of material was examined with no evidence to support that patients would be placed at significant risk or harm. The literature established that access to care via Direct Access arrangements improved patient satisfaction and dental care, as did the cost benefits to patients.
Consequently, the GDC Scope of Practice (SoP) document was updated to reflect the implementation of Direct Access in 2013. Accordingly, changes were made to Dental Hygienists’ and Dental Therapists’ ability to diagnose, prescribe and interpret radiographs and treatment plan within their scope.
An example of some of the changes following the implementation of Direct Access is illustrated below:
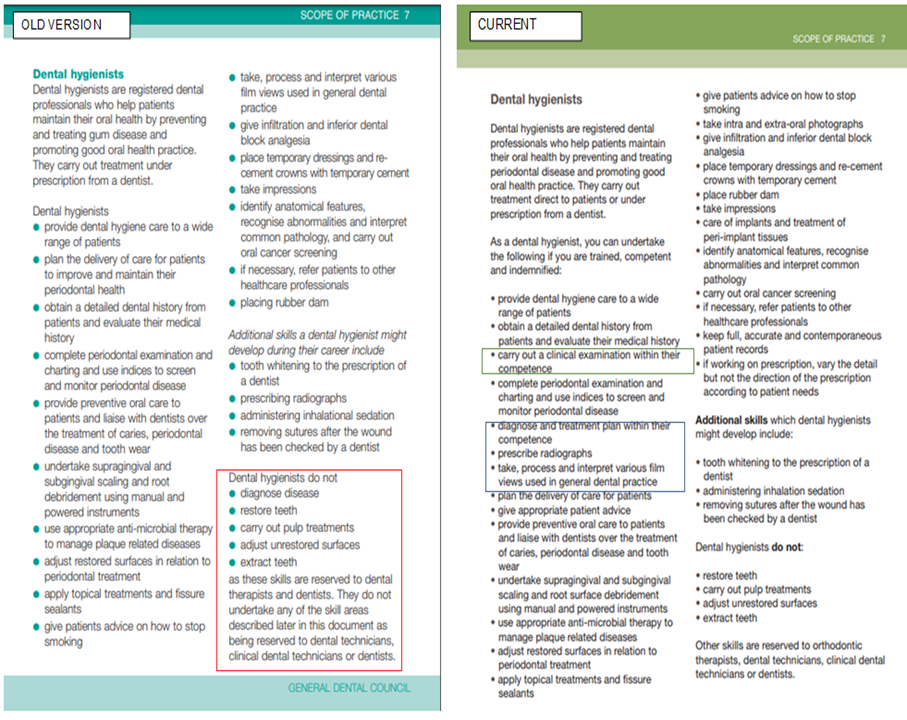
It is worth noting that the GDC is currently reviewing the 2013 SoP guidance and have already published findings from their research that started in 2019. The study was initially commissioned to help the GDC understand whether the document was being utilised as intended. The conclusions of the report highlighted unclear boundaries. Therefore, the GDC recently invited comments from several stakeholders, including dental care professionals, to engage and provide insights into the Consultation proposals to revise the GDC SoP guidance. Therefore, whilst the 2013 SoP was changed in line with the introduction of Direct Access, the profession will likely see further amendments in due course.
As well as the unclear boundaries identified amongst the GDC research, Dental Protection has received increased calls and requests for advice following the NHS dental contract reform, which has added to further unclear boundaries surrounding facilitating Direct Access for NHS patients and the roles and responsibilities in opening an NHS Course of Treatment (CoT) and submitting an NHS claim.
This article provides some context behind the confusion and acts as an update in sharing some of the concerns voiced surrounding Direct Access by our members.
Opening the doors of Direct Access for NHS Care
When Direct Access was introduced, the earlier research focused on patient safety and whether patients would suffer harm or be at an increased risk of a patient safety incident if they were allowed to access care directly from DCPs. There was little by way of a detailed review of The National Health Service (General Dental Services Contracts) Regulations 2005.
For example, The General Dental Service (GDS) contract confirms that a dental practitioner may perform dental services under the contract provided they are included in the Dental Performers List for a Primary Care Trust in England, and inclusion in that list is not subject to a suspension.
Applying to join the Performers List for England is only a requirement for General Practitioners (GPs), General Dental Practitioners (GDPs) or Optometrists who want to offer NHS services. Dental Hygienists and Dental Therapists, alongside other DCPs, do not fall within this requirement and are therefore not permitted under the GDS contract to submit claims for NHS treatment and was further supported by the FP17 Dental Forms only referring to dentists providing a course of treatment necessitating a Performer number.
Consequently, this led to an assumption that irrespective of Direct Access, DCPs could not see NHS patients directly because they were not admitted to the Performer’s List resulting in only private patients being given the Direct Access option.
However, NHS England began looking at ways to improve patient access to NHS care, and a closer look at the GDS Regulations highlighted a ‘widespread misunderstanding’ particularly concerning Part 4 of the GDS Regulations that refer to Persons Who Perform Services with the relevant provision shown below:

NHS England published guidance on supporting the use of skill mix and promoting the dental teams working together and more effectively to improve patients accessing care, seeking a legal opinion on the correct position about Direct Access from DCPs within NHS primary dental services. Following legal input and discussions with the GDC and the Department of Health and Social Care (DHSC), NHS England was satisfied “that dental therapists (DTs) and dental hygienists (DHs) can provide direct access to NHS care where that care is within the GDC scope of practice, if they are qualified, competent, and indemnified to do so” under the present GDS regulations.
Submitting an NHS claim for treatment
When details about the NHS Reform were first circulated back in July 2022, Dental Protection received numerous queries, and it highlighted a misconception amongst members and their dental teams that amendments to the GDS contract had taken place whereby Dental Hygienists and Dental Therapists were going to be added to the Performers List. However, the only change made to the GDS contract in removing the NHS barriers to Direct Access was an administrative amendment to the processing activity of the FP17 Dental Forms highlighted below.

Before October 2022, DCPs who had provided NHS care by referral and following a patient-specific prescription could not record their clinical contribution on an FP17. Following the abovementioned amendments, a facility immediately exists for DCPs to showcase their involvement in an NHS patient’s care using their using their own personal number recorded in the same field where a dentist’s personal number would go.
The NHS Business Service Authority (BSA) has provided guidance notes on completing FP17s and, through their Knowledge Base, offers additional information on submitting claims if a DCP has carried out all or part of a CoT.
Implications of Direct Access
Direct Access has allowed DCPs to work more independently without relying on supervision or a defined prescription from a dentist.
The GDC Direct Access guidance requires both dental hygienists and therapists to establish a system where treatment is needed, and the clinician feels it is beyond their scope or competence, must have an established pathway to refer those patients to a dentist or other relevant healthcare service or provider.
Whilst Direct Access increases autonomy, it also means that DCPs can be open to more scrutiny and investigation, primarily if they do not promptly refer patients to an appropriate dental practitioner. Therefore, it is advisable for any practice providing Direct Access to ensure that there is enough dentist capacity to accommodate the referrals.
Direct Access also remains a choice, and those who decide to work in this way must be confident they have the skills and competencies to treat patients directly. The GDC proposes that dental professionals consider spending a year post-qualification working under the prescription of a dentist, as many newly qualified DCPs will want time to gain confidence.
Working within your competency
Dental hygienists and therapists can carry out treatment for patients as part of a team, directly or under a written treatment plan from a dentist. They can conduct a clinical examination, diagnose and plan treatment within their scope of competence, and justify, take and interpret radiographs in compliance with the Ionising Radiation (Medical Exposure) Regulations - IR(ME)R 2017.
Page 43 of the Guidance Notes for Dental Practitioners on the Safe use of X-ray Equipment (2nd Edition) clarifies the roles of each registrant group.
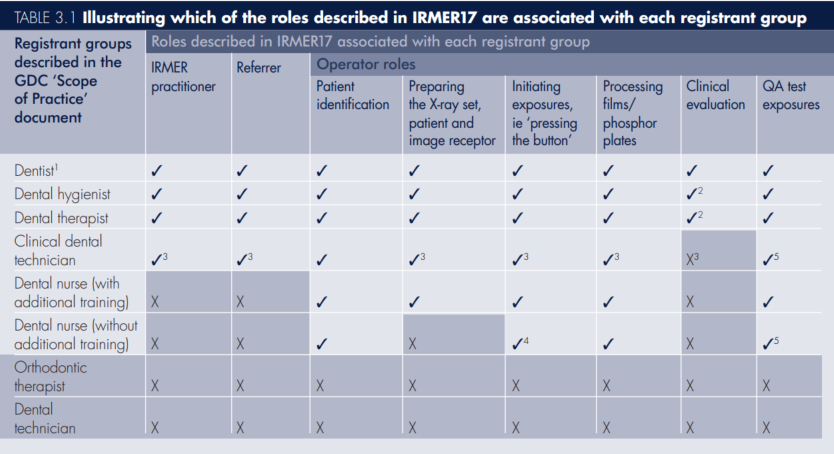
However, the GDC has advised that their SoP document is not intended to be an exhaustive or exclusive list of what registrants can and cannot do and that they expect registrants to use their professional judgement to determine whether they are appropriately trained, competent and indemnified for all duties they undertake.
The GDC have what it means to be trained and competent on their FAQs page and refer to...
“The best way to approach the concept of 'trained and competent is to ask yourself: 'If a complaint was made against me, how can I justify that I am trained and competent to carry out this particular additional skill?'
If you cannot confidently provide evidence to demonstrate that you are trained and competent, you need to think about whether you require more training or whether you could find some way to demonstrate your competence”.
With the above in mind, dental hygienists and therapists treating patients direct are expected to use their clinical judgement and know when and how to delegate and refer appropriately. This should be a reasonably simple handover in practices where a dentist works on-site. However, at locations where there is no dentist, there should be a precise and formal arrangement for the referral of patients, including the transfer of their clinical records and personal data. The referral process should be part of the practice’s standard operating procedure.
Dental Protection cannot advise specifically when a dental hygienist or therapist should refer a patient; they can only decide by using their clinical judgement, as explained above. For example, one DCP might feel something is beyond their scope, but another colleague feels the same treatment can be retained and performed in-house.
NHS and privately owned practices can offer patients Direct Access. However, only some surgeries will offer treatment via these arrangements. Equally, DCPs are not obliged to work under Direct Access arrangements, as confirmed via the GDC FAQ page.
Therefore, dentists should only direct colleagues to provide advice or perform treatment that falls within their competency with the current scope of practice of each DCP available here.
Do patients need to know they are being seen under the Direct Access arrangements?
GDC Standards 2 and 3 discuss the importance of ensuring a patient has all the information they need in a way they can understand to make an informed decision about their care. Therefore, a patient should be informed of a dental hygienist or therapist’s role and the potential limitations of a Direct Access appointment before booking. Practices don’t necessarily require a patient to sign a Direct Access form, as consent to treatment involves a two-way open discussion. Withholding information or failing to provide full disclosure to patients about their treatment has serious consequences. The Supreme Court ruling in Montgomery is a testament to that; therefore, any practitioner with a duty of care to a patient must inform material risks inherent in the proposed treatment. In doing so, consent is freely given whereby the patient and clinician mutually agree, not through medical paternalism.
Dental Protection has assisted with many complaints arising from poor communication or misunderstanding, so clear and concise communication for all appointments is paramount.
Prescription-only medicines (POMs)
The Consultation on the proposal for the supply and administration of medicines was published in October 2020. There were delays because of COVID-19, but submissions were made to allow Dental Hygienists and Dental Therapists to supply and administer specified medicines directly to patients under exemptions listed in Schedule 17 of the Human Medicines Regulations 2012.
After the Consultation ended, 2,743 responses were received from various organisations, including the General Dental Council, the British Dental Industry Association, the British Society of Paediatric Dentistry, and Community Pharmacy Northern Ireland.
The feedback from the consultation was very positive, with most respondents (97%) agreeing with the proposal to change the HMRs to permit dental hygienists and dental therapists to supply and administer medicines under exemptions.
Given the high level of support for this proposal, the UK government, jointly with the Northern Ireland Executive, progressed with UK-wide legislation to amend the HMRs 2012 and we saw The Human Medicines (Amendments relating to Registered Dental Hygienists, Registered Dental Therapists and Registered Pharmacy Technicians) Regulations 2024 come into force on 26 June 2024 to allow dental hygienists and dental therapists to supply and administer specified prescription-only medicines without the need for a prescription (or patient-specific direction or patient group directions.
Medicines for Administration can be found within the legislation above, through which the GDC welcomed this legislative change.
HOWEVER, whilst the legislation has been amended, training is required with the BSDHT advising…
‘While the change to the law means that you can administer specific medicines through exemptions from Human Medicines Regulations (HMR), this should only be done if you are trained, competent and indemnified to do so. You should not begin administering medicines via the exemption mechanism until you satisfy these requirements.
A curriculum for training has been developed by BSDHT and BADT and is owned jointly by both organisations. It is a requirement that prior to using this mechanism, you must access suitable education and training and it is advised that it follows this curriculum’.
The BSDHT also advises that NHS England is currently developing a course for Dental Hygienists and Dental Therapists. BSDHT and BADT will inform members when they are made aware of its availability.
Therefore, until then, if a Prescription-Specific Direction (PSD) and Patient Group Direction (PGD) are not present, a Dental Hygienist or Dental Therapist must not administer a Prescription-Only Medicine (POM).
Further information about the legislative changes can be found on the BSDHT website, and the impact assessment is available here.
Botox is a POM but, for obvious reasons, is not defined as one of the proposed medicines in the Consultation. Tooth Whitening, in any event, will remain under the Cosmetic Product (Safety) (Amendment) Regulations 2012, which draws a clear line between the products that can legally be used for tooth whitening by dentists or under their direct supervision. Direct supervision in this context means that the dentist must be on the premises.
What should a referral include?
The Faculty of General Dental Practitioners Clinical Examination & Record-Keeping Good Practice Guidelines is a valuable resource with Section 7 of the guidance highlighting several points to consider when referring...
“The referral, including options and reasons, should be discussed with the patient. The outcome should be recorded, and if referral is agreed it should be confirmed with the patient that this includes consent to provide relevant information for the referral. It should be discussed and noted as to whether the referral is on an NHS or private basis. A copy of the referral letter should be retained as part of the correspondence. However, it is not necessary to record that the patient gave consent as this is part of the process of referral”.
If referring by the NHS pathway, DCPs may find it helpful to review their local primary and secondary care providers’ referral criteria because each locality can vary in the measures that must be met.
Suppose a dental hygienist or therapist offers direct access care without a dentist on site. In that case, referrals of a different nature may also be required, such as safeguarding or potential oral cancer referrals. Dental teams can find up-to-date guidance and compulsory personal development on all potential referrals at Dental-referrals.org.
Indemnity
Finally, members of Dental Protection are entitled to request assistance with matters arising from their professional practice, and all requests are assessed individually. Dental Protection supports skill-mix and those dental hygienists and therapists wishing to provide treatment under Direct Access. Whilst we do not currently charge any additional fees to members working in this way, we ask that they make us aware if they are working under Direct Access arrangements to accurately reflect the variety of work volume and roles.
References
General Dental Council - Direct Access November 2020
General Dental Council - Scope of Practice 30 September 2013
General Dental Council - Becoming a dental hygienist or dental therapist 09 March 2022
NHS Building dental teams (2023)
Faculty of General Dental Practice UK (2016) - Clinical Examination & Record-Keeping 17 May 2016
RMSL & FDS Consultants - The Referral Process - https://dental-referrals.org/dentists/