The information within this article was correct at the time of publishing. However due to the fast-evolving nature of the pandemic, we strongly advise you to check all governmental and regulatory guidance for the latest updates.
The COVID-19 pandemic has created much uncertainty within dentistry. However, one important activity remains unchanged and is arguably more vital than ever. Elaine Cook, dentolegal consultant at Dental Protection, finds out why
A risk assessment is a systematic method of looking at work activities, considering what could go wrong, and deciding on suitable control measures. These control measures are designed to eliminate, reduce or minimise the risks of loss, damage or injury in the workplace.
Public Health Scotland
Dentists are well versed in undertaking risk assessments as part of health and safety for the dental practice. Indeed, it is a legal requirement for all organisations to carry out a risk assessment and, if you have five or more employees, you must also keep a written record. Although if you have fewer than five employees, it is still good practice to record for evidence of compliance.
However, the range of guidance, recommendations and advice that has been produced for practices on reducing the risk of transmitting coronavirus is unprecedented. It is therefore no wonder that many clinicians have been confused, stressed and even angry about how to reconcile all this documentation with getting back to work in their practice and the “new normal”. Nevertheless, detailed risk management approaches are now more important than ever to safeguard the health of patients and staff, and minimise the risk of infection. It is therefore essential that all dental practices undertake detailed risk assessments and look to mitigate the risks as much as possible.
Why are risk assessments still important?
In its May 2020 newsletter, the GDC said: “The process of determining whether it is safe will involve carrying out the necessary risk assessments and having regard to relevant guidance issued by professional bodies, the Government, other statutory bodies and the NHS.”
However, it is important to remember that we are still living through a unique and rapidly developing situation, which means there is a need for continual re-evaluation of the COVID-19 related risks as new evidence and guidance emerges.
There are five basic principles that apply when undertaking any risk assessment:
- Identify the hazard(s)
- Establish who might be harmed and how
- Evaluate the risks and decide on appropriate precautions
- Record and share key findings
- Review regularly
If this process is used systematically in each area of the practice, you will not go wrong. Areas to be considered include:
- Remote patient triage prior to attendance/COVID-19 assessment
- Outside the practice, the car park and the practice entrance/exit
- The reception area
- Waiting room
- Toilets
- Staff communal areas
- The treatment/operational environment
- Staff members individual risk assessments
- Clinic scheduling (AGP/non-AGP, vulnerable/shielding)
- Clinical records
- Infection control procedures
- Shift patterns and travel to and from work
- Laundry facilities
- CPR
What are the risks in dentistry?
Dental care providers have been considered to be at high risk of infection from COVID-19, owing to their face-to-face close communication with patients, exposure to saliva and blood during dental treatment, and due to procedures that generate aerosols.
Who might be harmed?
The obvious answer is the treating clinician, members of staff and the patient, but this could also include patient escorts or parents of young children who cannot attend alone and any contractors who may need access to the premises as well as those people living with any member of the dental team at home. Remember that special consideration should be given to those people who could be vulnerable or shielding and those who are at additional risk by virtue of underlying medical conditions such as high blood pressure, diabetes and being overweight, as well as pregnancy or ethnicity.
Evaluate the risks and decide on appropriate precautions
Usually when looking at a hazard we would assess the likelihood of it occurring and how severe its consequences might be.
The UK Government unveiled a five-level, colour-coded alert system on 11 May 2020 based on COVID-19’s reproduction (R) number, a scientific measure of how fast the virus is spreading and the number of confirmed coronavirus cases at any one time. Social distancing measures become tougher the higher the threat level is which invariably impacts on the working environment and the patient journey.
Every practice is different in respect of the premises, the staff and the procedures carried out, which means the measures taken will vary from practice to practice. How the guidance is applied is therefore down to each individual practitioner exercising sound professional judgement.
A hierarchy of control is a simple and systematic way to identify the most reasonable way to eliminate or reduce the potential for harm. Control measures utilised should be as high up the hierarchy of control as possible:
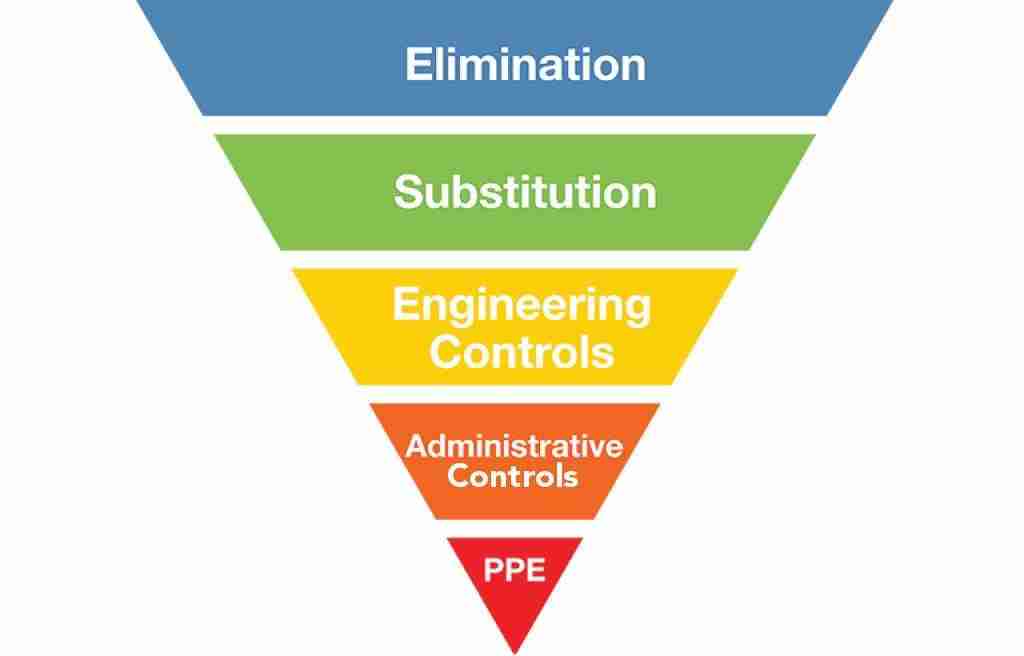
The risk of COVID-19 cannot currently be eliminated entirely but we can attempt to mitigate it.
Not all parts of the country are exposed to the same risk – we only need to look at the local lockdown measures implemented in Leicester in July 2020 due to a surge in COVID-19 cases for evidence of this – and regulators will expect practitioners to make their own competent assessment of the threat to their patients, their practice and their colleagues tailored to the circumstances at that time.
For example, you may choose not to do AGPs at all until more conclusive evidence about the risks emerge or all your staff are appropriately kitted out with the necessary PPE; or you could continue with telephone triaging and remote consultations, referring patients to a local urgent dental care centre until the COVID-19 alert level is reduced further.
The key to any risk assessment is justification for your decision and ensuring that this is appropriately documented. If you are in any doubt about specific risk control measures, discuss your options with our experienced team at Dental Protection.
Record and share key findings
This is absolutely crucial to ensure the whole team are aware of exactly what control measures must be followed.
During the COVID-19 crisis it is very likely that supporting documentation such as risk assessments would be needed to strengthen a clinician’s position if they were challenged in any aspect of the care they had provided. Any gaps or omissions are likely to be identified during any inquiry or investigation, and this will undoubtedly have an impact on the final outcome. In the unlikely event that your practice faces criticism, Dental Protection members should feel reassured that they can look to us for advice and support.
Review risk assessments regularly
You must regularly review your risk assessments to make sure that they are still valid. Staff risk assessments must be updated if there is a change in personal circumstances of the staff member (for example, the staff member notifies you that they are pregnant), or if there are changes in the working environment.
Consider appointing a COVID-19 lead who is responsible for regular reviews of risk assessments in line with the relevant current guidance, and encourage input from all members of staff. In the COVID-19 era it has become imperative for dental care professionals to keep themselves updated with the newest evidence-based guidelines, which are being revised faster than ever before.