In difficult times, we all look for ways to better manage ourselves and our staff. Considering the psychosocial safety climate of our practice is one helpful strategy that may in the past have been overlooked. Dr Annalene Weston, Dentolegal Consultant at Dental Protection, provides an overview.
When considering a new or unfamiliar concept, it is always helpful to start with a definition: “Psychosocial safety is the belief that you will not be punished or humiliated for speaking up with ideas, questions, concerns and mistakes.”
When contextualised as a workplace climate or culture, it is easy to understand that psychosocial safety could be an important workplace value. How important it is, or why it is important, is however easily overlooked in favour of seemingly ‘bigger-ticket’ items.
Why is it important?
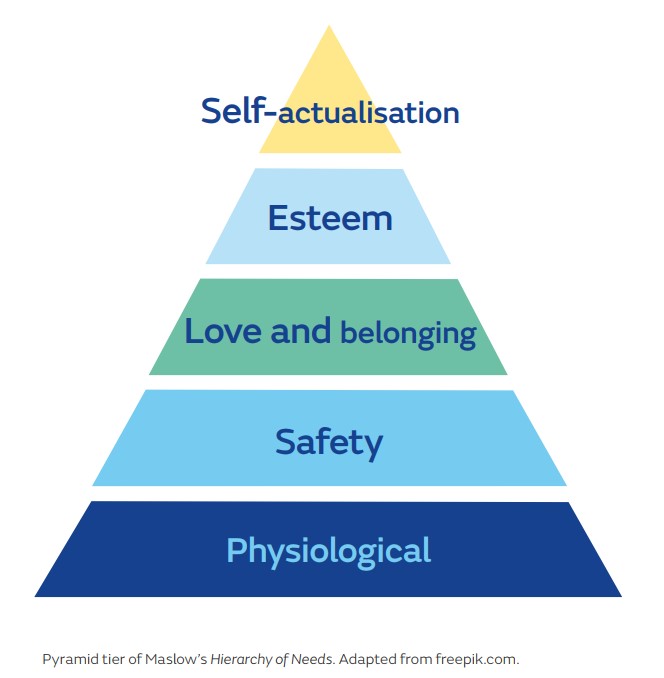
Maslow’s Hierarchy of Needs is a well-recognised concept that essentially highlights that basic human needs must first be met, if people are to achieve all that they are capable of.
If we do not feel safe in our workplace, for fear of ridicule or humiliation, or simply we feel we will not be heard, how can we feel safe at work? Naturally this feeling of discomfort would be compounded if we did not work in an environment with a no-blame culture, and mistakes are not forgiven but rather blame is apportioned between parties, appropriately or otherwise. Why would you ever speak up or voice a differing view if this was the reality of your workplace?
Somewhat alarmingly, if considered through to its natural end point, placing a barrier based in fear in front of a clinician or member of support staff will prohibit them from speaking up if there is a problem, or admitting an error they may have made. Errors in healthcare cost lives. And one thing we can all be sure of is that humans make mistakes, and we are all only human.
How do I make my psychosocial climate safe?
There are a number of strategies that you could consider implementing to improve the psychosocial safety of your workplace. Not only would this meet the basic psychosocial needs of your team and enable them to be the best version of themselves at work, but also it would serve to increase the likelihood that your colleagues and staff will bring their issues and concerns to you. Some simple strategies to implement tomorrow are described below.
As a leader or manager, you could consider encouraging a ‘no-blame’ culture, where mistakes and errors are seen as opportunities to learn rather than blame or label those who admit to their mistakes. A no-blame culture increases the likelihood of error being reported and decreases the likelihood these errors will be repeated, therefore improving patient safety and outcomes.
Another helpful strategy is to ‘ask’ rather than ‘tell’, and really listen to people’s responses. We are not all going to share the same views, and this will be more apparent than ever in divisive times such as COVID-19. Don’t make assumptions about how or why your staff or colleagues feel the way they do. Be curious, not furious, if their beliefs differ from your own. You may even learn something. And importantly, the act of listening without judgement will encourage that person to voice their concerns or opinions in the future, empowering a happier and safer practice.
Embrace a culture of mutual respect and civility, where differing viewpoints can be courteously discussed. Increased civility in the workplace serves to develop psychosocial safety and reduce the likelihood of bullying.
Finally, consider sharing your failures as opportunities to learn, not judge. Many are delighted to spruik their prowess, and engender the image that they are infallible, but the reality is that we learn more from our mistakes than we ever will from our successes. If we are open about our failures, and the lessons learned, not only do we entrench a culture where failure and error can be discussed without fear, but it also serves to give learning for all. Perhaps then, they will not need to repeat our mistakes.